Pulse Wave Velocity (PWV) is a valuable metric used to gauge the stiffness of arterial pathways, offering insight into the velocity of pressure waves within blood vessels. As the heart propels blood from the left ventricle into the aorta, pressure waves emerge. During the ventricular contraction (systole), blood ejection results in aortic wall dilation, triggering a propagating pressure wave across the arterial network. The movement's velocity serves as an indicator of arterial flexibility and compliance. Over time, vessels may experience increased stiffness due to aging or changes in their structural integrity, thereby accelerating the propagation of pressure waves.
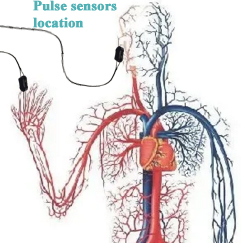
The PWV assessment involves the deployment of two pulse sensors positioned at a predetermined distance, constituting the Pulse Wave Distance. The temporal duration for a pressure wave to traverse from the upstream pulse sensor 2 to the downstream pulse sensor 1 gives rise to the Pulse Transit Time (PTT). Subsequently, PWV emerges from the mathematical division of distance by transit time, furnishing a gauge of cardiovascular health.
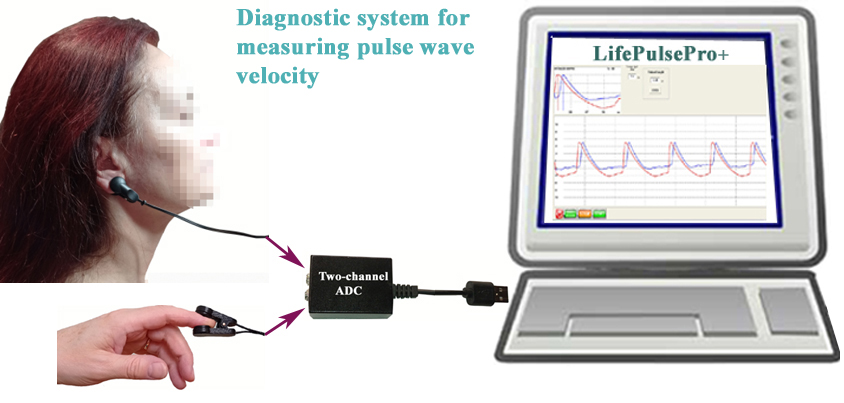
Introducing LifePulsePro+ an innovative advancement amplifying the pulse diagnostics domain through the integration of an auxiliary signal processing channel within the microprocessor unit. The incorporation of this secondary channel yields advantages and augmented functionalities, empowering an even more comprehensive and in-depth evaluation of the patient's overall health and physiological parameters.
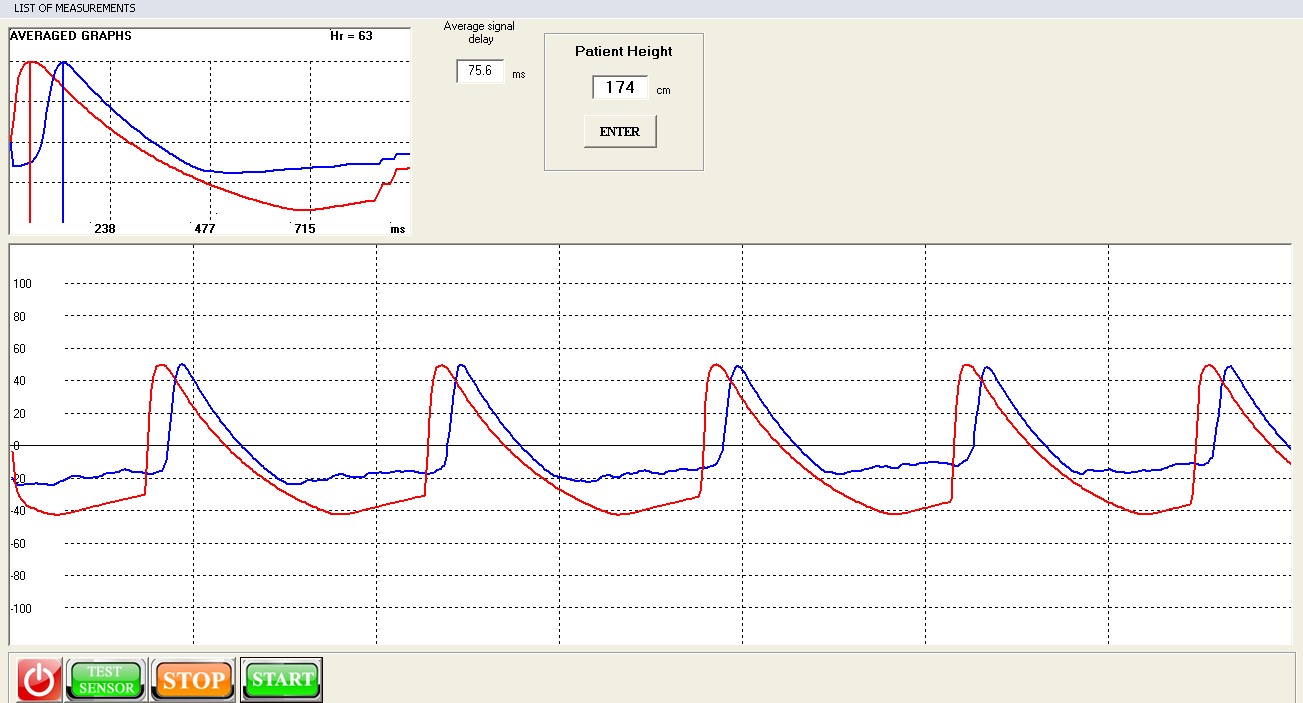
By harnessing the prowess of the supplementary signal processing channel, LifePulsePro+ adeptly handles concurrent data processing from a duo of pulse sensors. Positioned adeptly, one sensor graces the fingertip, while its counterpart resides affixed to the patient's earlobe. The PWM software module orchestrates the real-time capture and recording of pulse waves emanating from both sensors. Concurrently, the module quantifies the temporal delay encountered as the pulse wave traverses the vascular network, meticulously assessing this delay in milliseconds. Automated measurements unfurl seamlessly, culminating in the precise computation of the mean temporal variance in pulse wave amplitudes at two strategic measurement points.
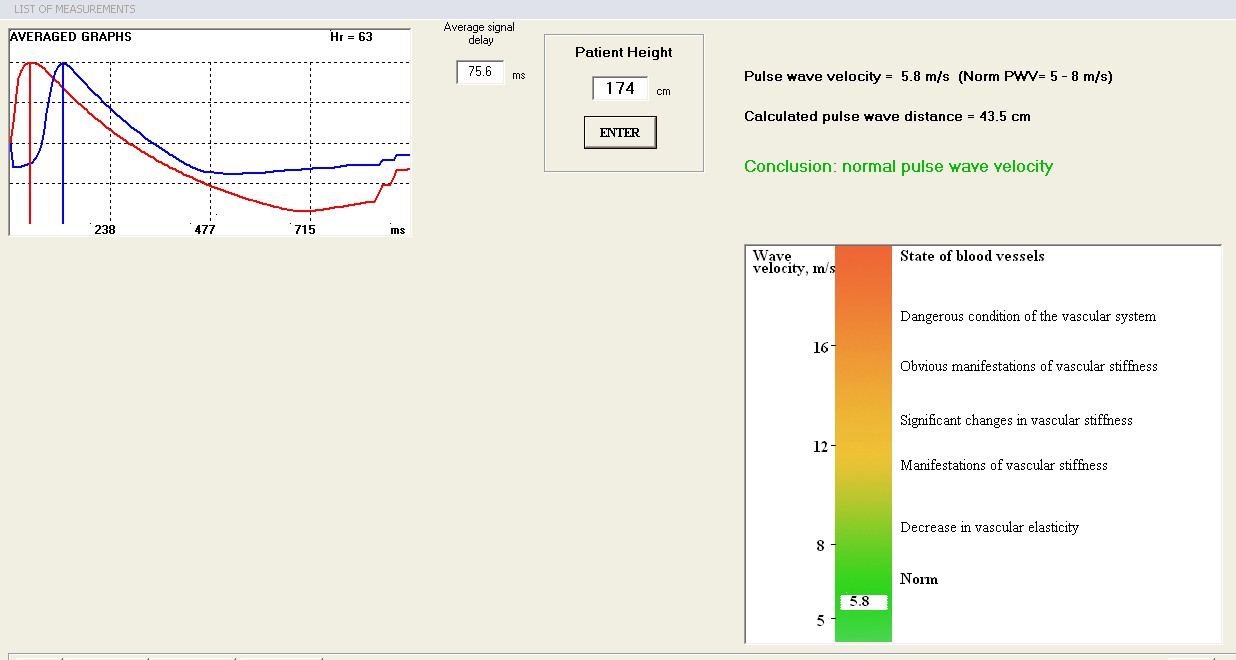
In the confines of the user-friendly dialog box, patients input their height, thereby precipitating the meticulous calculation of pulse wave velocity. A judicious calibration, accounting for signal delay, yields a comprehensive insight into the patient's cardiovascular dynamics. The synthesized analysis is subsequently presented in a visually informative manner.
The seminal analysis of pulse wave velocity stands as a classical hallmark, an index of vascular rigidity assessment. Notably, it emerges as a reliable harbinger, forecasting cardiovascular mortality within the hypertensive cohort. This prognostic value finds its fulcrum in the realization that the pulse wave velocity of vascular conduits is intrinsically interlaced with the passage of time, serving as a vital compass for deciphering the panorama of cardiovascular risk, particularly within the geriatric population.